PHLEGM67 | home
The Creed of the Air Force Society of Cardiopulmonary Technologists | MY RESUME | Acid-Base Physiology | On Mechanical Ventilation | The Winning Weaning Parameters | Original Articles and Views | Photo Album | Contemporary Cardiopulmonary Topics and Practice | Death and Dying Connection | Respiratory Care Boards and Committees | The Inspector's Corner - Regulatory Agencies | USAF Cardiopulmonary Society and AARC Affiliates | Breathe Sounds | Health Resources | Respiratory Publications and Articles | The Wheezer Connections - Asthma Etcetera | Youth Role Modelling and Respiratory Health Advocacy | On Becoming A Respiratory Case Manager | Whatever | Contact Me | House and Family Pixs
Original Articles and Views
METHEMOGLOBINEMIA IN HOSPITALIZED PATIENTS: A CASE SERIES
Sreekumar Subramanian, MD, Austin E. Delacruz, Jr., RRT, RPFT* and Rafaello Goeting, CRT, RCP. Departments of Surgery and Respiratory Therapy, David Grant USAF Medical Center, Travis Air Force Base California, USA
ABSTRACT
Purpose: Methemoglobinemia refers to the oxidation of ferrous(Fe2+) iron to ferric (Fe3+) iron within the hemoglobin molecule, which occurs following oxidative stresses. The subsequent impairment in oxygen transport may lead to progressive hypoxia and death. Early identification of this complication is often confounded by falsely normal diagnostic testing. The purpose of this report is to review the etiology, pathophysiology and clinical management of thisd uncommon, but highly dangerous condition.
Methods: The database of all arterial blood gas analyses at David Grant medical Center from 1998-2001 was reviewed to identify all patients with elevated methemoglobi levels (MetHb). % patients were identified with levels >10%. Their charts have been reviewed, with particular attention to any predisposing factors, treatment and clinical outcome.
Results: The mean methemoglobin level was 25% (normal 0-1.5%). In our series, topical benzocaine spray was the most common offending agent (4/5 patients). The reason for benzocaine use were: bronchoscopy/intubation (3 patients), and nasogastric tube placement (1 patient). In symptomatic patients, the threshold for instituting therapy is a level of 20% MetHb, with a lower threshold of 10% for patients with significant cardiac or pulmonary history. Asymptomatic patients generally do not require treatment for MetHb level less than 30%. The treatment of choice for acute, severe methemoglobinemia is intravenous 1% methylene blue, at a dose of 1-2 mg/kg
Conclusions: Methemoglobinemia is a rare complication encountered by various clinicians. Diagnosis requires a high index of suspicion, because pulse oximetry often gives near normal readings. Definitive diagnosis requires co-oximetry. Prompt treatment is essential to optimize outcome.
Clinical Implications: Early recognition of this condition, and administration of methylene blue can be lifesaving in severe cases.
File # 551412
Submitted for Presentation
CHEST 2002 Annual Meeting: American College for Chest Physicians
Presenting Author: Austin E. Delacruz, Jr., RRT, RPFT
Pulmonary Embolism Following Gastric Bypass Surgery at a Military Medical Center: A Retrospective Review
Sreekumar Subramanian MD, Austin Delacruz, RRT, RPFT, Rafaello Goeting, CRT, Departments of Respiratory Therapy and Surgery, David Grant USAF Medical Center, Travis AFB, California, USA
ABSTRACT
Purpose: Patients undergoing gastric bypass surgery for morbid obesity are at high risk for pulmonary and thromboembolic complications. Recent refinements in post-operative prophylaxis against pulmonary embolism (PE) may be responsible for improving patient outcomes. The objective of the present study was to document the prevalence of PE following gastric bypass surgery at our institution in order to better inform patients of the procedure's risk and benefits.
Methods: We performed a restrospective chart review of all patients undergoing gastric bypass surgery for morbid obesity at our institution from 1996-1999. Patient demographics, body-mass index (BMI), operative times, and the presence or absence of pulmonary embolism as a complication were recorded in a database, along with pertinent factors.
Results: 33 patients underwent gastric bypass surgery at our institution from 1996-1999. The mean BMI was 46 (Range 35-66). 5 of 33 patients (15%) were evaluated for pulmonary embolism with either V/Q scan, CT scan or pulmonary angiogram. 1 patient (3%) had a fatal PE diagnosed at post-mortem examination.
Conclusion: Pulmonary embolism is an uncommon, but potentially lethal complication following gastric bypass surgery. Meticulous attention to posoperative prophylaxis has reduced the rate of this complication.
Clinical Implication: Pulmonary embolism remains a source of mortality following gastric bypas surgery in a contemporary series of patients at a military medical center.
METHEMOGLOBINEMIA:
An Unusual Complication In Hospitalized Patients
Major (sel) Sreekumar Subramanian
TSgt Austin Delacruz, Jr, RRT, RPFT
SSgt Raffaello Goeting, CRT
Society of Air Force Clinical Surgeons
49th Annual Symposium
Las Vegas, Nevada 15-19 April 2002



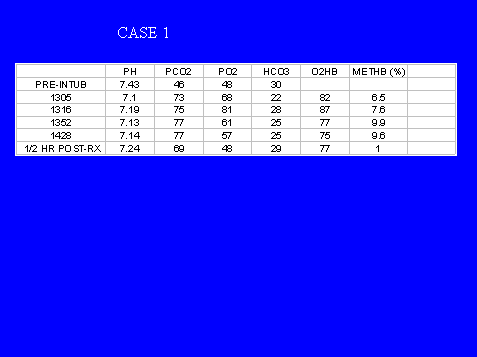

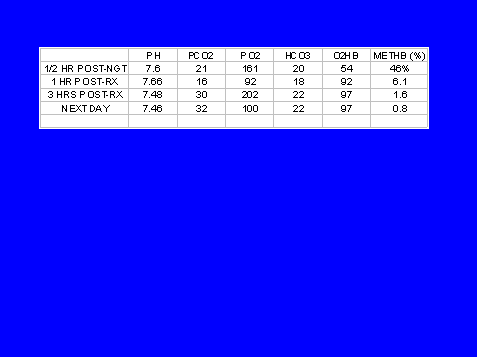

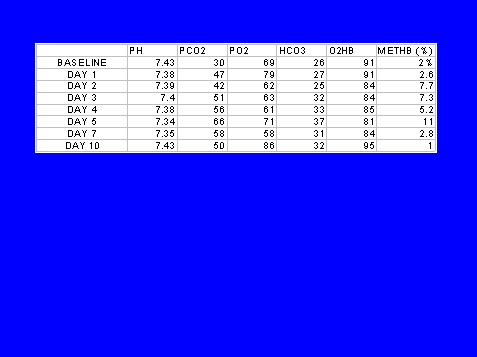








Full text in publication format available soon.
Ventilation with Lower Tidal Volumes as Compared with Traditional Tidal Volumes for Acute Lung Injury and the Acute Respiratory Distress Syndrome(ARDS): A Summarized Version Based from the Original Study
Introduction
This article evaluated the use of a lower then "traditional" tidal volumes in the ventilator management of patients with ARDS. A total of 861 patients are included in the study. They are evenly matched for relevant parameters such as age, sex, race and the severity of their illness. The four major causes of lung injury in the two groups were pneumonia, sepsis, aspiration and trauma, again evenly matched.
Study
One group of patients with ARDS on ventilatory support received "traditional" tidal volumes of 12 ml/kg of predicted body weight, the other matched group of patients with ARDS received lower tidal volumes of 6 ml/kg of predicted body weight.
Other variables such as ventilator mode, plateau pressure, allowable combinations of FiO2 and PEEP and oxygenation goal were standardized between the two groups.
Results
The study showed a decrease in mortality and a decrease in the number of days on a ventilator in the lower tidal volume group. The results were dramatic enough for the study to be terminated and the results published via the Internet.
The article notes the usual mortality from ARDS to be 40-50 percent. In this study the mortality rate for the "traditionally" treated group was 39.8% while the lower tidal volume group had a mortality of 31.0%. This is a 22% reduction in mortality in the lower tidal volume group.
Author's Conclusions
The authors attribute the improved survival rate in the lower tidal volume group to a reduction in excessive lung stretch in this group which caused less lung inflammation as measured by a lower interleukin-6 level in the lower tidal volume group.
The use of lower tidal volumes however, required treatment of the resulting acidosis with both increased ventilator rates and the use of intravenous bicarbonate.
The authors conclude: "On the basis of these results, high priority should be given to preventing excessive lung stretch during adjustments to mechanical ventilation, and this lower-tidal-volume protocol should be used with acute lung injury and ARDS."